Blood Groups: Types of Blood Grouping
Blood Groups: Types of Blood Grouping
The blood is classified on the basis of the presence and absence of antibodies and inherited antigenic substances on the surface of RBCs (red blood cells).
- The antigens may be proteins, carbohydrates, glycoproteins, or glycolipids, depending on the blood group system.
- Blood types are inherited and represent contributions from both parents.
Facts Associated With the Discovery of Blood Groups
Blood types were first discovered by an Austrian physician, Karl Landsteiner– an Austrian biologist, physician, and immunologist. He distinguished the main blood groups in 1900. He wrote a two-sentence footnote:
“The serum of healthy human beings not only agglutinates animal red cells but also often those of human origin, from other individuals. It remains to be seen whether this appearance is related to inborn differences between individuals or it is the result of some damage of bacterial kind”
- Karl Landsteiner classified human blood into three Blood Groups, namely Group A, Group B, and Group C.
- Landsteiner was awarded the Nobel Prize in Physiology or Medicine in 1930 for the discovery of blood groups.
- C was later renamed to O after the German Ohne, meaning without, zero, or null
- The group AB was discovered a year later by Landsteiner’s students Adriano Sturli and Alfred von DE Castello.
ISBT (International Society of Blood Transfusion):
The term human blood group system is defined by the International Society of Blood Transfusion (ISBT) as – A system in the human species where cell-surface – antigens- in particular, those on blood cells—are “controlled at a single gene locus or by two or more very closely linked homologous gene genes with little or no observable recombination between them.
As of 2020, the International Society of Blood Transfusion (ISBT) recognizes 41 blood groups.
What is an Antigen?
In immunology, an antigen (Ag) is a molecule or molecular structure, or any foreign particulate matter that can bind to a specific antibody or T-cell receptors.
- The presence of antigens in the body may trigger an immune response.
- The term antigen originally referred to a substance that is an antibody generator.
- An antigen can be proteins, peptides (amino acid chains), polysaccharides, lipids, or nucleic acids.
Blood Grouping System:
The two most important blood group systems are ABO and Rh, widely used all over the world. they determine someone’s blood type (A, B, AB, and O, with +, − or null denoting RhD status) for suitability in Blood transfusion.
ABO Blood Group System:
The ABO Blood Groups system involves two antigens and two antibodies found in human blood. These two antigens are antigen A and antigen B. The two antibodies are antibody A and antibody B. The antigens are present in the red blood cells and the antibodies in the serum.
Regarding the property of antigens in the blood, it can be classified into four groups,
- Antigen A with antibody B
- Antigen B with antibody A
- Antigen AB has no antibodies
- Antigen nil (group O) with antibodies A and B.

In between similar antigens and antibodies, there is an agglutination reaction – for example, antigen A agglutinates antibody A, and antigen B agglutinates antibody B. Thus, transfusion can be considered safe as long as the serum of the recipient does not contain antibodies for the blood cell antigens of the donor.
Table: Blood Groups and Donor Compatibility |
|||
| Blood Group | Antigens on RBCs | Antibodies in Plasma | Donor’s Group |
| A | A | Anti -B | A, O |
| B | B | Anti –A | B, O |
| AB | A, B | Nill | AB, A, B, O |
| O | Nill | Anti – A, B | O |
Blood transfusion:
Blood transfusion is a branch of haematology, it is related to the study of blood and blood groups. Blood transfusion compatibility is as follows:
Blood group AB:
The blood group AB shows the following features:
- The individuals have both A and B antigens on the surface of their RBCs, and their blood plasma does not contain any antibodies against either A or B antigens.
- Therefore, an individual with type AB blood can receive blood from any group (with AB being preferable), but cannot donate blood to any group other than AB. They are known as universal recipients.
Blood group A
Individuals with blood group ‘A’ show the following features:
- Individuals have the A antigen on the surface of their RBCs, and blood serum containing IgM antibodies against the B antigen.
- Therefore, a group A individual can receive blood only from individuals of groups A or O (with A being preferable), and can donate blood to individuals with type A or AB.
Blood group B
Persons with blood group ‘B’ shows the following features:
- The individuals have the B antigen on the surface of their RBCs, and blood serum containing IgM antibodies against the A antigen.
- Therefore, a group B individual can receive blood only from individuals of groups B or O (with B being preferable), and can donate blood to individuals with type B or AB.
Blood group O (or blood group zero in some countries)
Individuals with blood group ‘O’ show the following features
- These individuals do not have either A or B antigens on the surface of their RBCs and their blood serum contains IgM Anti-A and anti-B antibodies.
- Therefore, a group O individual can receive blood only from a group O individual but can donate blood to individuals of any ABO blood group (i.e., A, B, O, or AB).
- If a patient needs an urgent blood transfusion, and if the time taken to process the recipient’s blood would cause a detrimental delay, O-negative blood can be issued. Because it is compatible with anyone, O-negative blood is often overused and consequently is always in short supply
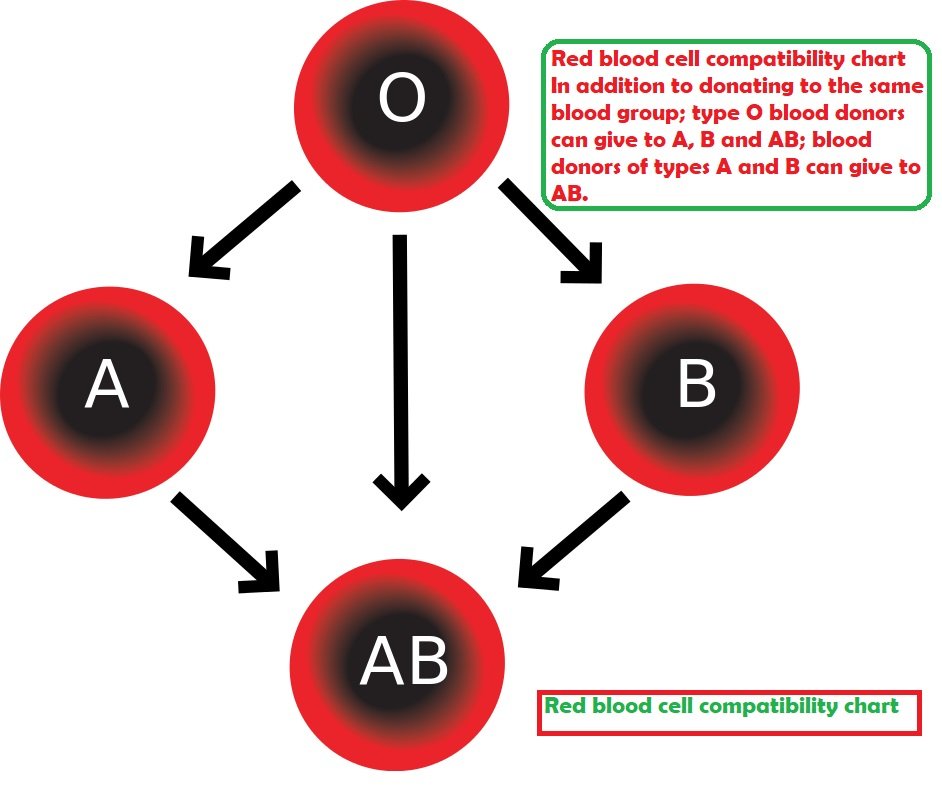
Universal Donor: individuals with type O Rh D negative blood are often called universal donors.
Universal recipient: Individuals with type AB Rh D positive blood are called universal recipients.
Blood compatibility test (Blood typing): The blood test is typically performed by the addition of a blood sample to a solution containing antibodies corresponding to each antigen. Agglutination indicates the presence of an antigen on the surface of cells.
Rh grouping:
It is the second most accepted blood grouping system after the ABO grouping system. The term “Rh” was originally an abbreviation of “Rhesus factor” founded by Karl Landsteiner and Alexander S. Wiener in 1937 in the rhesus macaque RBCs.
- Rh-positive: Individuals with antigen Rh on the surface of RBCs are called Rh-positive (Rh+ve).
- Rh-negative: The individual having RBCs without Rh antigen in the surface is called Rh-negative (Rh-ve)
If an Rh-negative person gets exposed to Rh-positive blood, specific antibodies against Rh antigens will be formed. The situation causes the death of the blood recipient. Therefore, the Rh should be matched for blood transfusion.
Erythroblastosis foetalis:
Erythroblastosis foetalis is a special case observed between the Rh-ve pregnant mother with Rh +ve blood of the foetus. Conditions occur as follows:
- In the first pregnancy, the Rh-ve blood of the mother does not get exposed to the Rh-positive foetus, as the blood of both is well separated by the placenta. However, at the time of delivery of the first child, there is a possibility of exposure of maternal blood to the Rh+ve blood of the foetus.
- In the case of exposure of maternal Rh-ve blood to foetus Rh-positive blood, the mother starts preparing antibodies against Rh antigen in her blood.
- After this, in her subsequent pregnancies, The Rh antibodies from the (Rh –ve) mother can leak into the blood of the foetus (Rh+ve), which destroys the foetal RBCs. This is fatal to a foetus or it could cause severe anaemia and jaundice in the baby. this condition is called erythroblastosis foetalis.
- This situation can be avoided by administering anti-Rh antibodies to the mother immediately after the delivery of the first child.
You can also read:
- Blood – definition, composition, and Function
- Circulatory system – Transportation
- Life Process-4 Excretion
Reference: https://en.wikipedia.org/wiki/Rh_blood_group_system#History
Thank you 🙂


1 Comment
Circulatory system - Transportation - PCSSTUDIES - Biology - · July 13, 2021 at 10:12 pm
[…] Blood Groups- Types of Blood […]